How a Hysteroscopy Can See and Solve Problems

Hysteroscopy is a medical procedure to identify and address various uterine and cervical conditions.
This enables the doctor to examine the inside of the cervix and uterine cavity visually.
How Can a Hysteroscopy See and Solve Problems?
A hysteroscopy is a medical procedure that enables the visualization of the inside of the uterus using a hysteroscope, a thin, lighted tube.
During a hysteroscopy, a specialized instrument known as a hysteroscope is utilized. This slender tube, equipped with a light source at its tip, is gently introduced into the vaginal canal, navigated through the cervix, and advanced into the uterus.
If abnormalities are identified, the physician can collect tissue samples for further laboratory analysis, assisting in the diagnostic evaluation.
This procedure serves both diagnostic and operative purposes, allowing healthcare professionals to see and address various gynecological problems.
Diagnostic Hysteroscopy vs. Operative Hysteroscopy
Diagnostic and operative hysteroscopy are two different procedures performed in gynecology to evaluate and treat conditions affecting the uterus. Here’s a breakdown of each procedure:
Diagnostic hysteroscopy identifies causes of abnormal uterine bleeding, aiding in the diagnosis of conditions such as abnormal endometrial thickening, postmenopausal bleeding, blocked fallopian tubes, endometrial cancer, intrauterine adhesions (scar tissue), and infertility.
Operative hysteroscopy is a surgical procedure using a hysteroscope to address uterine abnormalities. It’s recommended for conditions like abnormal uterine bleeding, fibroids, and other uterine disorders.
The surgery can include procedures such as endometrial ablation, septum resection, myomectomy, and polypectomy, targeting various issues in the uterus, cervix, and vagina.
A doctor might perform diagnostic and operative hysteroscopy in a single procedure to address identified issues without needing a separate surgery.
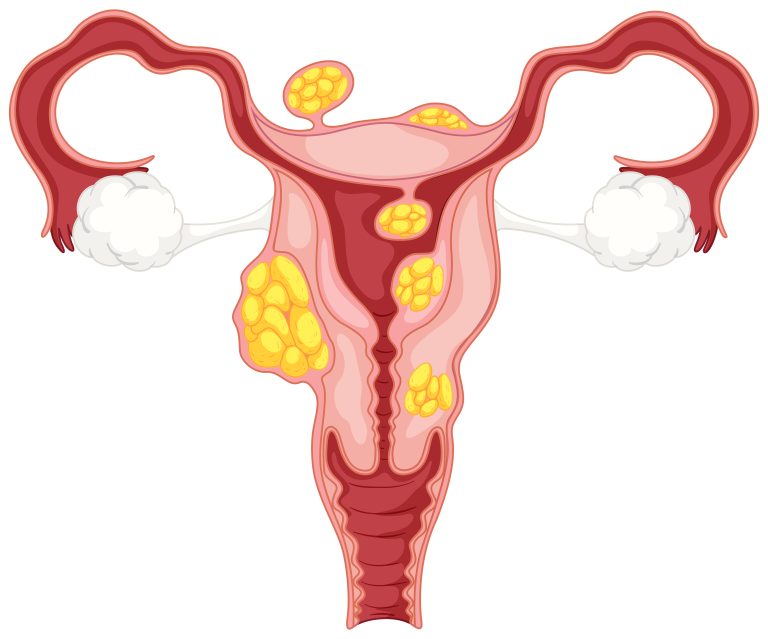
Reasons for hysteroscopy
One of the primary motivations for undergoing a hysteroscopy is the occurrence of abnormal uterine bleeding, a prevalent concern for many individuals. This encompasses experiences such as unusually heavy menstrual flow or bleeding episodes that transpire between regular periods.
The root causes of such irregularities often involve the presence of noncancerous growths within the uterus, such as fibroids and polyps.
A hysteroscopy is often conducted for women with repeated miscarriages to explore the causes. It is also employed to locate displaced intrauterine devices (IUDs), remove scar tissue from surgeries or infections, and establish fallopian tube blocks as a permanent contraceptive measure.
Hysteroscopy enables the collection of tissue biopsies for lab investigation, aiding in diagnosing endometrial issues and the lining of the inner uterine walls.
Hysteroscopy Procedure
Hysteroscopy can be done in a hospital or at a doctor’s office. It may involve local, regional, or general anesthesia. If under general anesthesia, you may need to fast for 6 to 12 hours. Medication and dilators help relax you, and a speculum is used to keep your vagina open.
The hysteroscope is carefully placed through the cervix, and either gas or saline is introduced to enlarge the uterus, providing a clear visual.
Images are displayed on a monitor. If treating conditions like polyps or fibroids, tools for removal are inserted through the hysteroscope.
For optimal timing, if you have regular periods, the first week after your period is recommended. However, it can be done at any time if you’re past menopause.
A hysteroscopy is avoided if you’re on your period, pregnant, have a pelvic infection, genital herpes, cervical or endometrial cancer, heart disease, or a tendency to bleed easily.
Inform your doctor if your period unexpectedly starts before the procedure, and avoid vaginal medicines, douches, or tampons 24 hours before.
How long does a hysteroscopy take?
A hysteroscopy typically lasts 5 to 30 minutes, occasionally extending to about an hour. The duration depends on the type of hysteroscopy, whether it’s diagnostic, operative, a combination, or part of another surgical procedure.
What is Laparoscopic Hysteroscopy?
Laparoscopic hysteroscopy is an advanced procedure merging hysteroscopy with minimally invasive laparoscopy, enhancing the diagnosis and treatment of gynecological issues.
This approach is especially practical for conditions like endometriosis or uterine fibroids, offering a more comprehensive solution.
Getting Pregnant After Hysteroscopy
For women considering gynecological procedures, fertility is often a key concern. Fortunately, hysteroscopy can enhance fertility by addressing uterine issues like polyps or fibroids.
Period After Hysteroscopy
Hysteroscopy can influence the menstrual cycle, causing changes like lighter or heavier periods and altered duration. These variations are usually temporary, resolving within a few cycles.
FAQs related to Hysteroscopy
Although hysteroscopy is generally safe, some women may face temporary bladder issues afterwards, like increased urination frequency or difficulty emptying the bladder.
These usually resolve within a few days, but it’s essential to stay hydrated and notify your healthcare provider if problems persist.
While infections post-hysteroscopy are uncommon, staying alert for signs such as fever, persistent pelvic pain, or unusual discharge is crucial.
After a hysteroscopy, your recovery depends on the anesthesia type. If under general anesthesia, you’re monitored until stable, needing a ride home due to impaired driving ability. Post-procedure, expect some cramping or bleeding.
Severe pain or heavy bleeding with fever is rare but requires immediate medical attention. Follow your caregiver’s instructions on abstaining from intercourse and avoiding feminine hygiene care, typically for about two weeks.
Post-hysteroscopy, frequent urination is common but temporary. The procedure may briefly irritate the bladder, causing increased urgency. Staying hydrated and giving time for irritation to subside usually resolves the issue.
Hysteroscopy pain varies, ranging from mild to potentially preventing procedure completion. Factors influencing pain include pre-procedure anxiety, duration, and childbirth history. Discuss anesthesia options and calming medications with your doctor for a more comfortable experience.
Post-hysteroscopy, the timeline for resuming activities varies. Typically, you may resume normal activities within a day or two.
Still, your doctor may advise delaying strenuous exercises, sexual activity, and tampon use for about a week to minimize complications and promote a smooth recovery.
Choose Dr. Sandesh Kade for Hysteroscopy in Dubai
Dr. Sandesh Kade is a highly regarded Gynaec Laparoscopic Surgeon with 22 years of experience globally. He specializes in minimally invasive laparoscopic, endometriosis, and pelvic floor repair surgeries, having performed over 10,000 procedures.
Dr. Sandesh’s expertise extends to fertility-enhancing surgeries, laparoscopy for fibroids, complex hysterectomies, and hysteroscopy for various conditions.


